HENDRA VIRUS (EQUINE MORBILLIVIRUS)
Ian Douglas
Manager, Emergency Response Capability
Animal and Plant Health Service
Queensland Department of Primary Industries
12 November 1999
The Hendra virus (previously termed equine morbillivirus, bat paramyxovirus or the cause of "acute equine respiratory syndrome") first became known when an explosive outbreak of respiratory illness associated with a high case fatality rate occurred in suburban Brisbane. Subsequently, horses have been found to have been affected on only two other occasions and a natural host has been found in the flying foxes or fruit bats (Pteropod bats). No standard bred horses are known to have been infected by the Hendra virus.
BACKGROUND
On 22 September 1994, an unusual syndrome associated with severe respiratory signs and death in thoroughbred horses was reported to the Queensland Department of Primary Industries. The initial report was received from a stable complex situated near to racetracks in suburban Brisbane. The owner of the stable complex was hospitalised at the time and a worker was ill. First signs of illness were noticed in horses that had competed on 17 September 1994. At the time this illness was attributed to recovery from racing. By the morning of 22 September 1994, two horses had been privately necropsied on the previous day, five other horses at the complex and one horse at an adjacent complex had died, and three horses were noticeably ill. Two other horses that had been moved from the stable complex were also seriously ill, one fatally. The owner died within a few days after a period on a respirator. Clinical signs reported included fever, severe respiratory distress, ataxia and swelling of the head, including the supraorbital fossa. Copious quantities of stable, sometimes red-tinged froth flowed from the nostrils in the terminal stages. The signs seen closely resembled the pulmonary form of African horse sickness, a viral disease that does not occur in Australia.
THE INVESTIGATION PROCESS
Post mortem examinations were immediately carried out on four recently deceased horses. Samples were submitted to the Australian Animal Health Laboratory (AAHL), Geelong to exclude the diagnosis of African horse sickness. Following exclusion, a detailed diagnostic process began. This involved description of the histo-pathological syndrome, and laboratory examinations that included virology, bacteriology, mycology and toxicology. A novel virus was isolated by scientists at AAHL and identical viruses were isolated from other horses by scientists at the Animal Research Institute, Yeerongpilly. The isolates originated from different horses, at two independent laboratories using different cell lines. Transmission trials at AAHL using first, crude tissue extracts and later, the supernatant from the virus cultures, reproduced a similar disease in experimental horses.
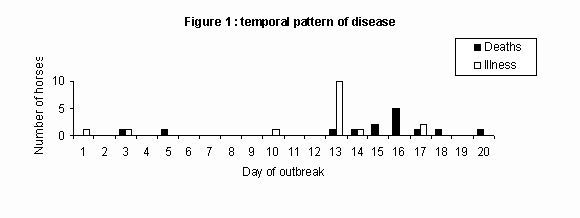
The index (or earliest) case was determined to be a pregnant thoroughbred mare that had been brought on 7 September 1994, noticeably ill, from a spelling paddock in a nearby suburb to the stables where she died two days later. The epidemic curve constructed at the time of the response appears below (Figure 1).

The incubation period of natural cases was mostly between 8-11 days with a maximum of 16 days. The mean time between onset of clinical signs and death was 2.1 days. Later it was shown that a total of 20 horses had been infected. Three of these had largely resumed a normal appearance following life-threatening clinical courses. Four other horses suffered mild illness. The seven surviving horses were euthanased to eliminate any possibility of disease transference from them.
The outbreak occurred primarily on a single stable complex of approximately 1000 square metres in area. The index case had moved to the complex two days prior to her death. Three infected horses had moved to two isolated properties soon after their exposure to the index case. Two horses resident in stables directly adjacent to the main stables were also infected. All infected animals had been held in close proximity to the index case. However not all horses were affected. Some of those maintained in the midst of affected stalls did not become infected.
Apart from the index case and an aged stallion, all affected horses could be classed as "horses in work". Mares and foals not routinely handled but held within the complex were unaffected. About two-thirds of all infected horses died as a result of their illness.
As this virus was new to the investigators, intensive follow-up was required to establish if the virus existed in the wider horse population. 5909 negative serological tests, including 4833 horse tests, were conducted between September 1994 and April 1995. Experimental challenge with the virus of a range of species was undertaken. A similar respiratory disease could be reproduced in cats and guinea pigs. The search for a natural host examined a wide range of other animals. Queensland Department of Primary Industries researchers found antibody able to neutralise the virus in flying foxes (fruit bats of the Pteropus genus). In September 1996, two years after the Hendra virus was isolated from horses, an apparently identical virus was isolated from flying foxes.
A SECOND FOCUS
A third human case (a second human fatality) was diagnosed in October 1995. This diagnosis was investigated and a second focus of infection was found on a rural property over 800 kilometres north of Brisbane. Retrospective examination of preserved tissues found that two thoroughbred horses at pasture were infected with the same virus. These horses had died in August 1994, approximately six weeks prior to the outbreak described above. A renewed effort to find further evidence of the virus in Queensland failed to demonstrate any further infection in the horse population.
A THIRD FOCUS
On 18 January 1999, north of the coastal city of Cairns, a single thoroughbred mare died suddenly and was subsequently shown to be affected by the Hendra virus. This mare was at pasture and had been used for polocrosse. She had only contacted one other horse during the previous six months and this horse, when subsequently tested, showed no indication of infection with Hendra virus.
DISCUSSION
The three foci have no known connection in terms of common stock, equipment or transport. The identification of the flying fox as a natural host may provide the explanation for these three apparently unconnected incidents.
Studies provide strong evidence for establishing that the initial Infection spread from the index case in each of the first two outbreaks to other horses and to three humans.
Australia has invested heavily in contingency planing for exotic animal diseases to protect its advantageous disease status. This process has led to the development of the Australian Veterinary Emergency Plan (AUSVETPLAN). This plan includes specific disease strategies for known threats but also describes approaches for investigations and responses that are generic in nature and can be applied to most situations. The procedures detailed in AUSVETPLAN are also applied successfully to emergencies that arise from outbreaks of endemic diseases.
The outbreak of the Hendra virus (bat paramyxovirus) sparked an interest amongst scientists and captured the imagination of media agencies throughout the world. The virus has been restricted in its occurrence but has shown itself as the cause of severe disease in horses and humans. Intensive surveillance within Queensland since 1994 (including retrospective examination of many years of laboratory records) has resulted in only three occurrences being identified.

It seems clear that the Hendra virus is not a virus of horses but under extremely unusual circumstances it is able to "spill over" to cause disease in horses. While it spreads widely among flying foxes, it has been transmitted only with great difficulty to and from horses.
|
|
|
|
|
|
|
|
|